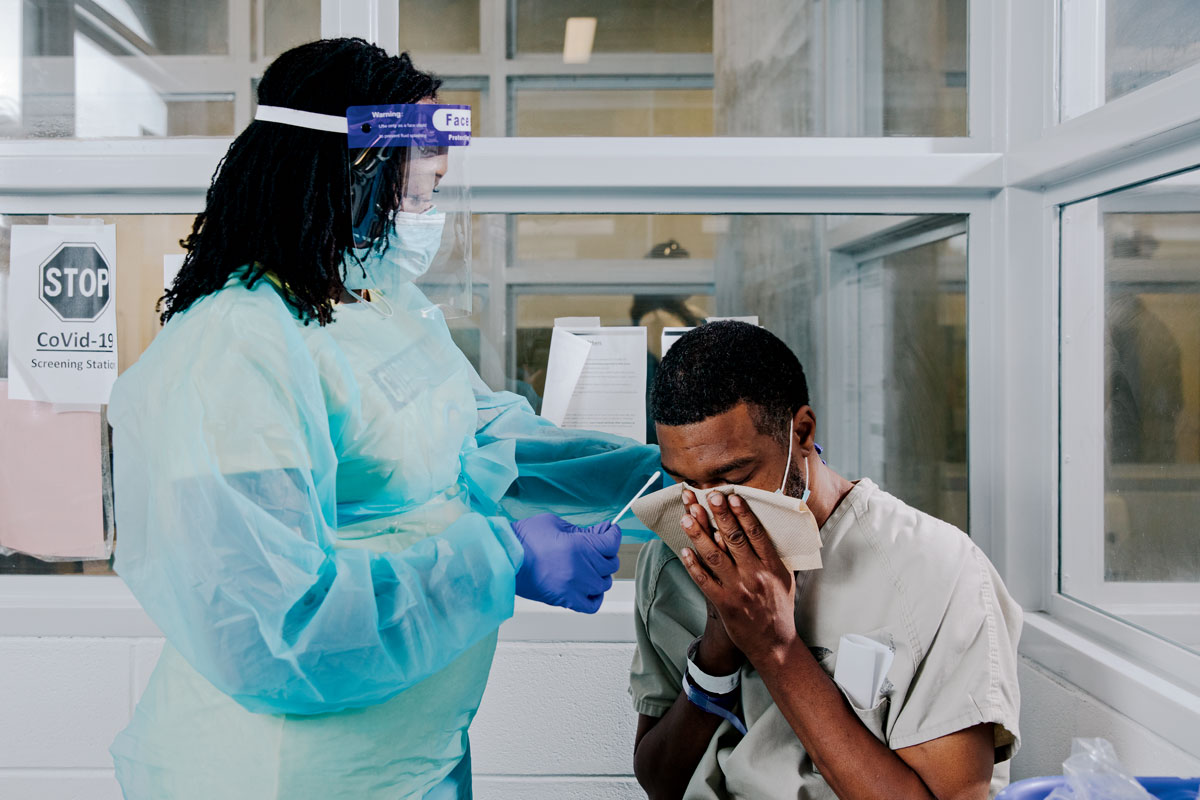
As the last days of January fled, the skyline of the country’s largest single-site jail knuckled up against a cold, chalky sky, its slab walls and watchtowers thrusting upward like fists, making it look like a forbidding junior college campus. The man who runs Cook County Jail, Sheriff Tom Dart, likens it to a small town. There’s the population: some 5,000 inmates on any given day and 2,400 staff members. There’s the size: The collection of soot-smudged limestone and brown brick buildings stretches across 96 acres and eight city blocks on the southern edge of Little Village, looming grimly over the neighboring bodegas and bungalows. And then there are the services: The jail has a medical center, a privatized food provider, a commissary, multiple classrooms and chapels, and a transport system — the blocky white buses and the vans that roar in and out of the site daily.
But in every other important and defining way, it is not a town at all. The residents are captive, of course, and held in tight quarters. Some stay in the “dormitories,” large rooms filled with rows of bunk beds. Others are doubled up in 6-by-10-foot cells on two-floor tiers that can hold as many as 48 inmates each. Each tier has a single common space: a medium-size room with bolted-down tables and a wall-mounted TV.
Though built to confine, Cook County Jail remains, under normal circumstances, a hive of activity, fed by a steady influx and outflow of people. In 2019 alone, nearly 60,000 people awaiting trial or bond release passed through, charged with everything from trespassing to triple murder. The newly arrested are herded, shoulder to shoulder, into the basement, where they are clumped 20, 30, 40 at a time in various chain-link holding areas as they are processed. Add to that the hundreds of lawyers, contractors, and suppliers who come and go, plus the 500 to 1,500 people visiting inmates each day.
All of this — the captive population, the close quarters, the constant flow of people — makes the place a petri dish, as Cook County Board president Toni Preckwinkle called it, a place particularly susceptible to the rapid spread of a contagious disease. Indeed, from mid-March through April, COVID-19 “turned the jail upside down,” Dart says, leading to 1,000 cases among inmates and staff in that span alone. Ten people — seven inmates and three correctional officers — would eventually die from the disease. The jail would be declared the “top U.S. hot spot” by the New York Times. It would be hit by a federal class-action lawsuit on behalf of inmates that alleged Dart failed to stop a “rapidly escalating public health disaster” and demanded he do more. Protesters would line up outside calling for the jail to release all its inmates.

Yet it could have been worse. The jail would ultimately be praised by the Centers for Disease Control and Prevention for controlling the contagion inside its walls at a time when it continued to spread outside them. Dart would claim victory, proclaiming at a news conference that “we not only bent our curve, we killed off the curve.”
Since there were no established guidelines for him to follow, Dart’s efforts did not always go smoothly. Still, he managed to react on the fly, adjusting his hastily created plan, sometimes with prompting from the courts, to mitigate the disaster — what the CDC report would call “one of the largest outbreaks of COVID-19 in a congregate setting.” This is the inside story of what happened.
In the waning days of January, with COVID-19 having landed in the United States after already engulfing central China, Dart grew worried. He began seeking a plan that addressed what to do in the event of an outbreak in the jail. “I was dying — dying — to get someone to give me a playbook, for someone to say, ‘Here, Tom, here you go. Just run it out.’ ” He looked to major cities with expansive incarceration systems and to the Large Jail Network, an information clearinghouse for sheriffs and jail administrators. But he found “nothing anywhere” for dealing with such a serious contagion.
In early March, after Seattle became a hot spot, one of his staffers reached out to someone at the King County Jail there who had connections to Chicago, trying to get some insight. “They have no idea what they’re doing,” Dart remembers his staffer reporting back. “They’re just trying to figure it out.” At that point, Dart says, he realized “we were left to our own wits to come up with a plan.”
The jail was fortunate in one sense: Its annual battle against the flu meant it had a set of protocols for dealing with widespread illness. “We just went back to those basic practices,” says Dr. Connie Mennella, chair of correctional health at Cermak Health Services, which is responsible for treating inmates at Cook County Jail. That meant reemphasizing hand washing and sanitizing frequently touched surfaces. It also meant reminding “officers to be on alert for symptomatic inmates so that if you see someone coughing or sick, put a mask on them, get them isolated,” she says.
While Dart and Mennella were trying to mobilize, the seriousness of the virus’s spread was revealing itself in increasingly dramatic ways in the outside world. On March 9, after Illinois confirmed its 11th case, Governor J.B. Pritzker issued a statewide disaster proclamation. That day, the jail began its version of sheltering in place, reducing rehabilitative programs for inmates and restricting movements around the campus. Two days later, the NBA announced that it was suspending the rest of its season. For Dart, the reality hit full force when he saw footage of Thunder and Jazz players leaving the court as the crowd watched in stunned silence. “I don’t want to say that’s when I first took it seriously. But when I saw the NBA, just before the start of the game, cancel like that, I was like, OK, what’s going on here?”

Dealing with the steady influx of new inmates — each a possible carrier — was paramount. “I had about 200 new people entering the jail every day for bond hearing purposes,” Dart says, “and we were holding on to 60, 70 percent of them.” He called for temperature checks on all new inmates beginning March 13. (The jail had been asking them screening questions about international travel and flu-like symptoms since late January.) Any new inmate showing signs of the disease were sent to the jail’s residential treatment unit, where they were given a mask. Starting March 20, Dart would order the other new inmates kept isolated for 10 days before being allowed to enter the general population. (Later, on April 16, after the jail opened up more housing, the isolation period would be extended to 14 days.)
Visitations were tricky too. The easy solution would have been to simply suspend them. But that would’ve hurt morale. For many inmates, some of whom have been locked up for years awaiting trial, such visits were “the only thing keeping them mentally able to deal,” Dart says. “I knew if I cut the visits, tensions would rise in the divisions.” He had been having visitors’ temperatures checked since March 13 and had limited the number of people on each inmate’s visitor list to two, but he worried that wasn’t enough. “As things were ramping up,” he says, “I was like, No, I gotta end it.” He did so on March 15. To soften the blow, he provided inmates with more free phone calls. “I also got moving on video visitation. That’s just a very difficult thing to hardwire. But we did it.”
Dart also worked to curtail the daily movement of inmates to and from hearings and trials. He knew that every bus trip between the jail and the courts in suburban Markham, Bridgeview, Maywood, Rolling Meadows, and Skokie, with inmates seated side by side, put everyone involved at risk. “Guys, we can’t keep doing that,” Dart says he told the judges. “There’s no reason we can’t do this via teleconference or Zoom or whatever.” The courts eventually set up an online system in which defendants, with their lawyers, could be arraigned and participate in hearings, but getting buy-in “took a little bit of pushing on my part because the courts weren’t in a full shutdown mode yet.”
Even with those efforts, Dart and Mennella realized they wouldn’t be able to shut out the virus entirely. “Once COVID had hit the city, we knew it was only a matter of time before it entered the jail,” says Mennella. “We were bracing for impact. I don’t think we realized at the time how hard it would be.”
That impact began March 18. An inmate reported having shortness of breath and a fever. When his flu test came back negative, the jail isolated him and notified the Chicago Department of Public Health of a possible coronavirus infection. The staff at Cermak wanted him to be tested for COVID-19 right away, but because he had not traveled internationally and had no known exposure, he did not meet the CDC criteria at the time. (Widespread testing of symptomatic inmates wouldn’t begin until March 25.) Cermak sent specimens to the CDC anyway. The test results arrived 10 days later, confirming what the staff already assumed: COVID-19 had officially arrived at 26th and Cal.
The situation now more urgent, more tough decisions had to be made. One of those came on March 23, when Dart halted programs for inmates entirely. Another critical issue was how to reduce the jail’s population, which stood at just under 5,600. In the 14 years Dart had been sheriff, the once notoriously overcrowded jail had cut its population by half, but it remained plenty congested.

Advocate groups were already demanding the immediate release of medically vulnerable — if not all — inmates. But Dart did not have that authority. “It’s not like I could wave a magic wand and let everyone go. I’m the one holding everybody, but I’m the one with really the least amount of ability to do anything about it.” Still, the need to reduce the population was undeniable. Dart worked with the offices of the Cook County state’s attorney and public defender, firing off lists of candidates for release, nonviolent offenders in for property crimes and DUIs. Eventually, these efforts would reduce the jail population to about 4,900.
But that alone wouldn’t be enough. Dart knew he also had to find more housing to better spread out inmates (he began converting cells to single occupancy on March 26) and to isolate the infected. Inventorying the facilities, Dart identified several unused floors and buildings to convert to housing.
Even before the virus hit, the jail had managed in only three days to repurpose a cluster of buildings just outside the main campus. Those four structures — three of which could house as many as 80 people — had once been used for a boot camp program offered to first offenders as a way to avoid probation or a jail term. No one had lived there for several years. “I’d been using it to treat the mentally ill,” Dart says. “I was like, We’ll convert that into dormitories” and use it to put people who tested positive for COVID-19, but had milder cases. “I saw how this thing was going and that I needed a place to put people who were sick where they can be monitored somewhere away from the jail.”
Readying buildings that had been mothballed for years in such a short period of time proved a major logistical undertaking. One needed a new roof. All needed fresh paint and a thorough disinfecting. Heating and cooling systems had to be repaired. And to create even more space, Dart installed four large, military-style canvas huts at the site.
By March 16, the converted boot camp was ready for use (though the first inmates would not be placed there until March 30). All told, Dart now had an additional 500 beds at his disposal. That would relieve some of the pressure on the residential treatment unit and the medical center. Critical cases, such as those requiring ventilators, would continue to be sent to Stroger Hospital, St. Anthony Hospital, and other nearby facilities.
Dart was preparing for the worst, and in late March, the number of infections among inmates began to jump. On March 24 alone, there were 20 new cases. The next day saw 65, as the Cermak staff began testing asymptomatic inmates, beginning with the most medically vulnerable, in units where there had been exposure. By the end of March, 199 inmate cases would be confirmed. The numbers were rising among the staff members too, with the total hitting 34 by month’s end.
With the situation growing more dire, Dart was still flying blind. “We were just grinding,” he acknowledges. “Just making it up.” He was concerned enough about catching the disease himself that he sent his wife and kids to his mother’s summer house in Indiana out of fear of transmitting it to them. “I literally didn’t see them for three weeks,” he says. “I spent Easter at my house by myself, eating frozen food.”

As the numbers rose, Lenzie, an inmate who asked to be referred to only by his middle name, felt a sense of unease bordering on panic growing in himself and among his fellow inmates. A year earlier, he had been arrested after police found a gun in a van in which he was a passenger. He insisted the weapon belonged to the driver, and planned to argue that when he went on trial. Now he hoped he was not facing a death sentence from the pandemic sweeping through the jail. “Everybody [in the country] was freaked out, but we were more scared than anyone because we couldn’t go nowhere,” he says.
With the media reporting alarming developments each day, Lenzie says, crowds grew around the jail televisions: “Usually, you would have maybe 10 guys in the dining room watching TV. When news [of COVID-19] hit, you would have like 48, 49 guys. Once they started to explain more about it and then they began to shut down activities [at the jail], we knew it was serious.”
If Dart and Mennella were doing all they could, Lenzie says, he wasn’t seeing the evidence. “We were still two to a cell. And they weren’t cleaning the way they should — mold in the shower, mold on the wall, it just being nasty, you know?” (Dart’s office points out that inmates are responsible for cleaning their own cells and most other areas of the jail, though it’s the role of correctional officers to inspect these locations.)
In late March, before Dart ordered guards or inmates to wear masks, Lenzie and other inmates improvised, he says. “We started making our own. Different types of cloth — T-shirts. You gotta be a person with some type of imagination in jail, you know?” But almost as soon as the homemade masks appeared, Lenzie says, they were confiscated. When I asked, the sheriff’s office denied that was the case. “We are unaware of any instance where staff confiscated masks made by detainees to protect themselves from COVID-19,” it said in a statement.
On April 2, Dart finally ordered his staff to wear surgical masks, but it would be another 11 days before all inmates would get them. One reason for the delay, Dart says, was the mixed messages he was receiving from the CDC, which didn’t start recommending that the public wear masks until April 3. It took additional time, he says, to stock enough masks so that inmates and staffers could get fresh ones each day, in accordance with CDC recommendations.
Lenzie, who was released on electronic monitoring on March 26, wasn’t the only inmate with concerns. On April 3, the law firm Loevy & Loevy, the nonprofit Civil Rights Corps, and Northwestern University’s MacArthur Justice Center filed a federal class-action lawsuit on behalf of the jail’s inmates, alleging that Dart had failed “to take appropriate steps to curb the substantial threat posed by COVID-19.” The lawsuit demanded, among other things, that anyone with underlying medical conditions be released immediately and that additional preventive measures be taken.
“The Cook County Jail is being overrun by COVID-19,” Stephen Weil of Loevy & Loevy said in a statement at the time. “Currently, the infection rate inside the jail is nearly 40 times the overall rate in Cook County. And while the rest of us have been able to engage in social distancing to protect ourselves, both detainees and jail staff alike have alerted us that numerous people inside the jail, many with serious medical conditions, are housed in open areas where social distancing is impossible.”
The lawsuit also alleged that Dart’s claims about the steps he was taking amounted to little more than PR. “We had a lot of facts about what was happening on the ground that contradicted the sheriff’s narrative,” says Alexa Van Brunt, an attorney with the MacArthur Justice Center. That evidence came from affidavits filed on behalf of 69 current and just-released inmates.
One inmate, for example, Sean Alexander, told his girlfriend that he was still sharing a cell, and that after one inmate on his floor tested positive and was removed, the jail staff put that man’s cellmate in with someone else. “That person is now coughing and jail staff have told him not to touch the remotes and keep in his cell,” the girlfriend said in her statement given April 2. She also said Alexander told her that he and his cellmate had to buy cleaning supplies from the commissary because the jail wasn’t providing it. Dart refutes that, noting he was going to great lengths to make sure inmates had enough bleach and disinfectant. He says he waived a long-standing rule against the use of hand sanitizers, instituted because some inmates had used them to start fires.
Soap was another issue. Several inmates stated in their affidavits that they weren’t getting enough and that the bars they did get were tiny hotel-size ones. Dart counters that there is good reason the jail stopped providing larger bars: Some inmates were stuffing them in socks and using them as weapons. In one case, an inmate used a makeshift flail to kill another. That said, “they have soap,” Dart says. “And we know they have soap.”
Two days after the federal lawsuit was filed, as Dart’s lawyers were preparing a response, the jail recorded its first COVID-19-related death. Jeffrey Pendleton, a 59-year-old inmate with a string of gun and drug charges as well as a 1997 rape conviction, died after a six-day battle with the virus. Pendleton had a number of underlying conditions, including pulmonary heart disease, hypertension, and several past cases of pneumonia. Soon Pendleton’s brothers filed a lawsuit alleging that Dart kept their brother shackled to his hospital bed, even while he was hooked up to a ventilator, causing him excruciating pain and violating his constitutional rights.
Both lawsuits caught the attention of the media. But it was an April 8 article in the online edition of the New York Times — its headline proclaiming Cook County Jail the “top U.S. hot spot” for the virus — that generated a public relations nightmare. The jail, the story declared, was “the nation’s largest-known source of coronavirus infections … with more confirmed cases than the U.S.S. Theodore Roosevelt, a nursing home in Kirkland, Wash., or the cluster centered on New Rochelle, N.Y.” The article came out just as the number of COVID-19 cases at the jail was hitting a peak. In one five-day span, from April 6 to 10, the jail saw 227 confirmed cases — more than half of them guards. A day after the Times story went up, a second inmate, Leslie Pieroni, died of COVID-19 complications.
Not only did the story shine a harsh spotlight on Dart and the jail, it sent inmates into a full-blown panic. “We were listening to their phone calls,” Dart recalls. “We could hear them talking to their family members, literally saying, ‘I’m going to die. I heard this is the top hot spot. I’m going to die in here.’ ” Inmates posted handmade signs in the windows: “We Matter 2.”
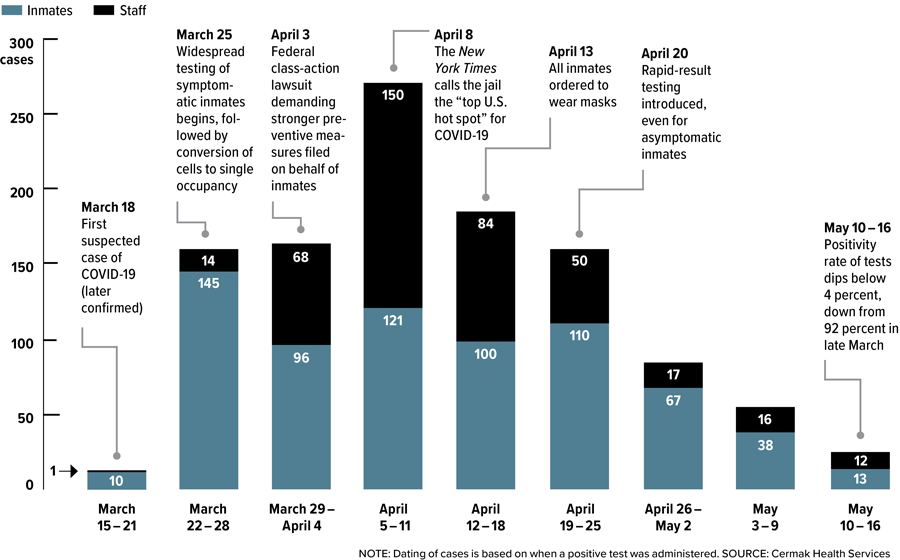
Cook County Jail’s “Public Health Disaster”
That’s how an attorney who filed a federal class-action lawsuit on behalf of inmates in early April described the jail’s COVID-19 surge. But a combination of preventive measures and more and better testing largely beat back the outbreak by mid-May.
Tap to view larger
Dart was livid at the portrayal. Yes, the jail’s numbers were comparatively high, he argues, but that was because at the time the jail was one of the few institutions doing testing — and making the results public. “Here I am trying to manage this and working around the clock with my staff — no one is sleeping,” he recalls. “I was just infuriated because it was clearly misrepresenting what was going on. That we were still having issues with it wasn’t because we were being indifferent to it. We were trying everything. I felt like, If you have a better idea of what we can do, please let us know and we’ll try that.”
The article, he says, was “devastating” for staff morale. And in the days after, Mennella’s medical crew had to walk past protesters gathered outside the jail shouting, “Murderers!” “They were so unnerved,” Mennella told Dart of her staff, according to the sheriff. “I was having to calm them down, to explain that they needed to just ignore that.”
The day after the story came out, the judge overseeing the federal lawsuit granted a temporary restraining order that gave Dart until the following Monday to implement testing of all symptomatic inmates and to eliminate the use of “bullpens” — the large cages where people who have been arrested are assigned while they await their bond hearings or jail intake processing. The judge also ordered Dart to ensure that inmates had enough soap and cleaning supplies and to make masks available for all symptomatic inmates.
To this day, Dart vents his frustration over having had to siphon time and resources from the jail to attend court hearings for demands he felt he was already meeting. He had, for example, already opened up several new housing areas and was putting as many inmates as he could in their own cells. His staff was being provided masks, and he was already working on finding enough for inmates. “So we go through that whole thing that didn’t need to be done to be ordered to do everything that we’re already doing,” Dart says.
By mid-April, the efforts seemed to be working. The numbers began to drop. Dart and Mennella hoped they had turned a corner, but then came another wave: 160 in a weeklong span from April 19 to 25. On April 19 alone, three people, including the first correctional officer, died from COVID-19-related causes. The next day, another inmate died, bringing the total deaths at that point to seven.
Dart was mystified. “We were trying everything we could to put the brakes on this thing. We were going back and looking at everything, looking at patterns, like, Is there any commonality here? Was there something we missed?”
On April 27, the judge overseeing the federal lawsuit said that Dart had to do more in the way of social distancing. Specifically, he ordered that, with some exceptions (such as units where everyone living there was being treated for COVID-19), inmates could no longer be housed two to a cell and that Dart must ensure that every inmate had a mask as well as regular replacements. By this time, Dart says he had largely already accomplished both, though he had not yet, as the judge also ordered, lowered the number of inmates housed in every dormitory by 50 percent.
As it turned out, the crucial factor — perhaps the single most important in the jail’s finally getting a grip on the outbreak — had been Cermak winning approval from Abbott Laboratories to be one of the first sites to use a new rapid test the pharmaceutical giant had developed. With it, results were available within a few hours, rather than days, making it easier to segregate infected people. Previously, because of the delay, it had made little sense to test asymptomatic inmates on a more widespread basis.
After Cermak starting fully implementing the new test on April 20, new cases soon dropped off dramatically. May 5 was the last day the jail registered double-digit positive tests. And the number of inmates in isolation with COVID-19 dropped from a high of 307 in early April to less than 100 by May 21 to less than 20 by late June. Meanwhile, the infection rate — that is, the percentage of tests that came back positive — plunged from more than more than 90 percent in late March to about 1 percent by mid-June, a rate that has remained relatively steady to this day, even as the jail’s population has crept back up to its pre-COVID-19 levels of more than 5,000.
That quick turnaround shows how a “timely response can reduce case counts and prevent morbidity and mortality in correctional or detention facilities,” read the CDC report also authored by various county and city offices and made public in July. In short, the report held up Cook County Jail as a case study in how to handle such an outbreak, citing “complex and resource-intensive interventions,” each “critical and timely.” For Dart, the report is vindication.
Mennella says she appreciates the praise, particularly given the harsh criticism, but points out that the fight isn’t over. “We must remain vigilant.” Even now — with plenty of masks and cleaning supplies, and infection rates far below the general public’s — she closely monitors the inmates who are being treated to make sure they are doing their part. “I was in a division the other day,” she says. “I saw masks hanging at the chin, so I had to sort of gently say, ‘Guys, we want to keep you safe, but you have to do these things’ — reminding them about social distancing and hand washing and wearing the masks properly. Just like in the community, when complacency sets in is where you can run into problems. We want to make sure that we’re still on high alert.”
In mid-June, Matt Walberg, spokesman for the Cook County sheriff’s office, and Salomon Martinez, superintendent of one of the jail’s housing buildings, led me on a tour of the facility, a walk-through via FaceTime (Walberg had offered an in-person tour, but out of an abundance of caution we settled on a virtual version). By then, the situation at the jail had improved so much that Dart has reinstated visitations, holding them outside — provided the visitors were willing to wear masks and have their temperature checked.

The hallways the two men walked, normally bustling with lines of inmates heading to eat, to programs, to court appearances, were as empty as a college campus over spring break. Walberg offered to show me any area I wanted.
At one point, Martinez paused when I asked him about inmates’ allegations that they did not have cleaning supplies. Like Dart, he vehemently denied the claims, saying that the facility was cleaned so often with so much bleach that it had “begun to smell like a swimming pool.” In one case, he said, paint was literally scrubbed off a wall. He pointed out large jugs of hand sanitizer he said were filled every shift. “We go through six gallons every couple of days.”
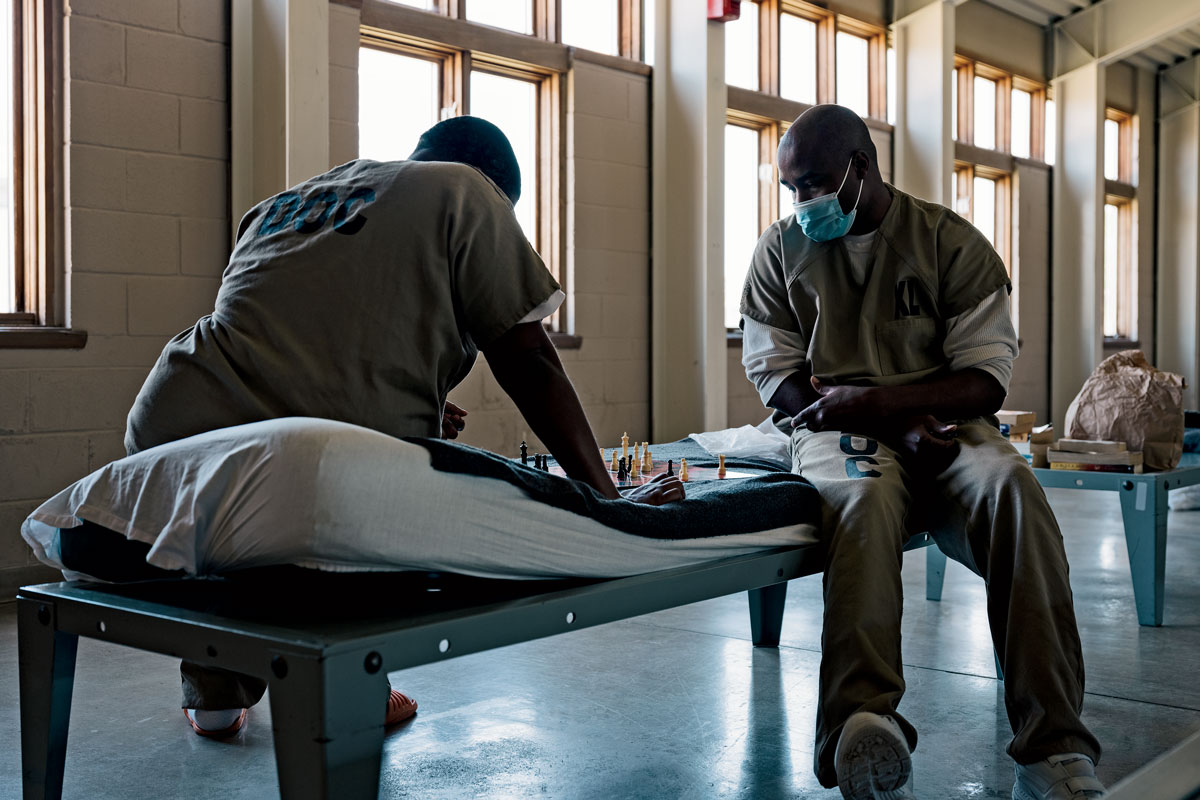
I was also shown a “day room,” an open area ringed by two floors of cells. On one wall, a television flickered, watched by a few men at tables bolted to the floor, where every few feet or so was a marker indicating the proper social-distancing lengths. “We used to allow 48 inmates out at a time,” Martinez explained, peering through a window at the inmates. “Now it’s 12.”
I could see that not all of the men had masks on and a few were probably sitting too close to one another. Martinez says the jail tries to monitor mask wearing as much as possible, but as in the outside world, there are some people who simply refuse to comply. The only leverage the staff has, he says, is taking away perks like phone use or free time granted to walk the shared spaces.
Walberg concluded the tour by showing me around the converted boot camp. All was quiet. The grounds, as well as the collection of buildings and huts, were mostly, if not completely, empty, a ghost town compared with the main jail campus.
There wasn’t much to see. Walberg pointed his phone camera into one of the four buildings, which was filled with bunks. I was then shown the huts, each outfitted with beds, the kind you might see in army barracks. The structures had air conditioners, but the units were never turned on.
In the end, for all the scrambling to provide extra beds, less than 200 of the 500 at this location were ever used.
It struck me that despite the fact they were largely unused, the buildings stood in mute testament to how bad things could have gotten and how unsure people were, and still are, of where and when it all will end. It was an awful lot of work, though, I mused, for seemingly naught. True, Walberg said. But nobody, of course, was complaining.
The Dead
Over the course of less than 12 weeks, seven inmates and three correctional officers at the jail died from COVID-19 or related complications.
Jeffrey Pendleton
Inmate, 59
April 5
Pendleton was being held on a string of gun and drug charges and had been convicted in the 1995 rape of a Hyde Park doctor. He died within a week of being diagnosed. Citing Pendleton’s chronic health issues and age, public defenders had argued for his release just before his death. “He wasn’t as bad as people think. He just had issues,” his brother Warren told the Chicago Tribune. “I don’t think anybody should die like that.”
Leslie Pieroni
Inmate, 51
April 9
A resident of Rogers Park, Pieroni was awaiting trial on a 2018 charge that he had sexually assaulted a boy under 13. He had been hospitalized since April 3.
Nickolas Lee
Inmate, 42
April 12
Held on armed robbery and gun charges, the South Shore resident had been sick for two weeks. His wife, Cassandra Greer-Lee, says she made more than 130 calls to the sheriff’s office trying to get help for her husband. Since his death, Greer-Lee has regularly organized protests outside the jail. “I don’t want this agony on anyone,” she told ABC-7.
Karl Battiste
Inmate, 64
April 19
Accused of killing a man outside his apartment building in South Chicago, Battiste had been held without bail since January 2019. He called his daughter Karla on Easter Sunday to say his head was hurting. Just a week later, he would die at Stroger Hospital. Karla says her father had noticed the spread of symptoms in his hall and that his bed was under a vent. She was never formally notified of her father’s death, getting the news from a family member weeks later. “He was the smartest guy I ever knew. I could call and ask him a question about anything and he knew the answer,” she says. “I wasn’t ready for him to pass like this.”
Rene Olivo Sangabriel
Inmate, 42
April 19
Since October, Sangabriel had been held without bail on aggravated drunken driving charges. In early March, his attorney opted to keep him at Cook County Jail rather than enter a plea so the Little Village resident could finish his addiction treatment program. Undocumented, Sangabriel apparently feared that leaving Cook County Jail would put him in the “arms of immigration,” a niece told the Tribune. “He wanted to wait there.”
Sheila Rivera
Correctional officer, 47
April 19
The former social worker and police officer had worked at the jail since 2012. A diabetic, she tested positive two days before her death. “She liked helping people,” her brother, Sonny Mattera, told CBS-2. She is survived by her husband, Noland, a Chicago police officer, and a 16-year-old son.
Juan Salgado Mendoza
Inmate, 53
April 20
Held on charges that he stabbed a woman in the neck during an argument in Cicero in November 2018, he had been hospitalized for a week.
William Sobczyk
Inmate, 53
May 4
Sobczyk had been treated for advanced cancer at the jail before being transferred to Stroger Hospital on April 18 for COVID-19-related complications. Held for his alleged involvement in a Northwest Side bar fight, he was due for a hearing the day after his death to reevaluate his bail due to his health issues.
Antoine Jones
Correctional officer, 51
May 10
The South Side resident and grandfather of seven had worked at the jail since 2002. A diabetic, he had been diagnosed with COVID-19 six weeks before his death. “The virus just took him down. He had to go on dialysis, his kidneys shut down, everything just shut down on him,” his wife, Sylvia, told ABC-7. He eventually died of cardiac arrest.
Jose Pedro Marquez
Correctional officer, 52
June 28
A correctional officer since 2004, he lived in Berwyn with his wife. He was a father of five and grandfather of three.














Comments are closed.