
Doug Waldron, back on track after facing what could have been the end
At first, Doug Waldron thought he had a cold. It lingered for a few months and settled into a constant cough, causing some pain on one side, in his upper ribs. “When I was younger, I had had pleurisy, and this was what it felt like,” says Doug, now 72, a retiree who lives in Round Lake Beach, 50 miles north of Chicago. “Like a cold that had gotten worse and settled in my upper side.”
“Every day I would ask him if he’d called the doctor, and every day he’d say, ‘No, I’m going to be all right. It will go away,’” recalls Doug’s wife, Diane. Finally, she made an appointment for him. During the exam, Doug’s internist thought he heard some congestion in his lungs, so he ordered a chest x-ray. The x-ray showed a faint dark spot on one lung, and Waldron was referred to the Condell Medical Center in nearby Libertyville, where a CAT scan was performed.
The first scan accidentally caught the top of Doug’s liver, and to the surprise of the Waldrons—and that of the technicians, as well—it revealed what appeared to be a tumor. “The doctor called us and said now there needed to be a scan of his liver,” recalls Diane. “And he also said that we should know that something serious was probably going on here.”
The second scan was performed at the Condell Medical Center, and by the time the Waldrons were walking back into their house later that day, their phone was ringing with the results: The tumor in Doug’s liver was extremely large, about ten inches in diameter. More tests, including outpatient biopsies, were scheduled. Those revealed stage four liver cancer. The dark spot on Doug’s lung was a separate kind of cancer, less advanced and less immediately life threatening than the liver cancer.
The liver cancer, the Waldrons were told, was a medically dire situation. “When I heard that, I just walked out of the doctor’s office,” says Doug. “I didn’t want to know any more. I already knew enough.” Diane was well aware of her husband’s other medical challenges: He had diabetes, glaucoma, and collapsing veins in his legs, which limited his ability to walk. He smoked and was overweight. She pressed the doctor to give her an unvarnished prognosis. Chemotherapy was out, she was told. The tumor was too large. The doctor believed that Doug had about a month to live.
That nightmare diagnosis was made in July 2006. Today, more than two and a half years later, the Waldrons sit around their dining-room table drinking diet soda, shooing away their dog, and reveling in the unexpected outcome of Doug’s illness. Life is good these days.

Team players: The doctors Mary Mulcahy and Riad Salem were crucial members of the group that treated Doug Waldron at North- western Memorial Hospital.
“The liver tumor is gone, and this is what we call a wow outcome,” says the oncology radiologist Riad Salem in a phone interview. Salem is the director of interventional oncology at the Robert H. Lurie Comprehensive Cancer Center at Northwestern Memorial Hospital in Chicago. The Waldrons’ determination to search for the most advanced medical treatment that suited their case illustrates how even the worst diagnosis can sometimes be overcome. Interventional radiology is a subspecialty practiced at major academic medical centers, and Salem treated Doug’s liver cancer with radio- embolization—a new technique approved by the FDA in 2000. North- western is now the world’s busiest center for the treatment.
“I live and breathe these kinds of treatments, and so I know how extraordinary the good end result Doug got is,” says Salem. “The term ‘cancer-free’ is a difficult term for us, as physicians, to use. But it has been two years now, and he has no tumor in his liver, no tumor in his lungs. No signs of cancer at all.”
The Waldrons met in California and soon moved to Muskegon, Michigan, where Doug worked in an office-furniture factory, and they married in 1970—Diane had a son from a previous marriage, and Doug had three children. When Doug retired in 1990, the Waldrons moved to Tucson, Arizona. They liked the sun, and the dry heat agreed with them. But when one of their sons started working in Chicago, he urged them to move to this area. “He would say, ‘You’re not getting any younger, and if something happens, you are going to need help,’” recalls Diane. So the couple sold their Tucson home and moved to a pleasant two-story house beside a park in Round Lake Beach.
When Doug was diagnosed with cancer, they felt that the time for help had come. But at first, they couldn’t find any. They visited several oncologists and cancer specialists, looking for a treatment plan. “One wanted to talk about taking vitamins and finding my spiritual path,” says Doug. “Others said they couldn’t do anything for us,” Diane adds. Finally, the oncology specialist in Libertyville, Dean Tsarwhas, referred the Waldrons to Mary Mul-cahy, an oncologist at the Robert H.
Lurie Comprehensive Cancer Center. “I pull the medical team together to review what our options and limitations are,” says Mulcahy. “In a complicated situation like this, we do a lot of talking, both with the patient and with the team as we decide how to proceed.” Two days later, the Waldrons went to Northwestern Memorial Hospital.
“I thought we would be meeting with one doctor there,” says Diane. “But instead we were led into a conference room, and all these doctors and their nurses came in to discuss Doug’s case.” It was decided that the first step was up to Mulcahy and Salem. “I specialize in complex cancer therapies,” Salem explains. “The idea was if I could do something for the liver, then maybe we could move on and consider doing something for the lungs.” Salem has bachelor’s and medical degrees from McGill University in Montreal and an MBA from George Washington University; he has also held a fellowship at the University of Pennsylvania in Philadelphia.
Photography: Tom Maday
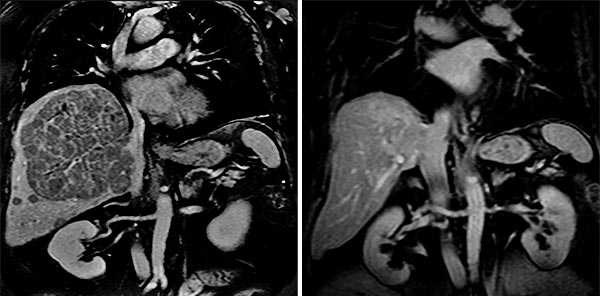
Then and now: The CAT scan on the left shows the tumor in Waldron’s liver soon after it was discovered; in the image on the right, several months after advanced treatment, all signs of cancer were gone.
The treatment that Salem proposed was an innovative therapy with yttrium 90 microspheres. A leader in this therapy, Northwestern has performed about 1,500 treatments. Salem has worked with yttrium 90 microspheres for ten years, treating patients referred to him from as far away as Hong Kong, and Northwestern Memorial has published about 50 percent of the medical literature on this treatment. The therapy, indicated for patients with inoperable liver tumors and other tumors that have spread to the liver, uses tiny radioactive spheres to attack cancerous tumors in the liver; yet the impact on the patient’s healthy tissues in general is minimal.
“It is a very sophisticated, very potent form of radiation,” says Salem. “We place a catheter through the groin up into the liver, and we inject these microspheres. When you think about normal radiation therapy, the patient lies there, and the machine tries to focus on the tumor for radiation. But it’s treatment from the outside in. For this microspheric treatment, you go on the inside to the tumor, and you inject the radiation directly into it.” The micro-spheres are directed through radiologic imaging, and patients receive usually only one treatment, sometimes two.
Salem delivered six million micro-spheres of radiation to Doug’s liver. Then the wait began. “It takes several months to see what the results are,” Salem says.

The aftermath: Waldron at home with his wife, Diane. “It’s a funny thing to say,” he explains, “but it was a very good experience.”
The road to recovery wasn’t smooth. Shortly after his radioembolization treatment, Doug became very ill and ran a fever up to 103 degrees. Northwestern didn’t have any beds avail-able, so Doug was transported from his home by ambulance to the Con-dell Medical Center. On the way, he suffered a mild heart attack. In this situation, doctors would normally have prescribed heart medication and exercise. Due to his poor circulation as a consequence of diabetes, however, Doug was unable to exercise. After he recovered from the heart attack, his team of doctors at Northwestern inserted stents into one of his legs to increase circulation. That dramatically increased his mobility. “At first, Doug would walk a few extra yards,” says Diane. “Then he could walk to the end of the driveway. Then he could make it around the park in back of our house.”
Still, a month after Doug’s micro-sphere treatment, Salem saw no change in the tumor in his liver. “It looked like there had been no improvement whatsoever,” says Salem. “I was a little disappointed.
In fact, I even gave him the ‘This therapy didn’t work for you’ speech. Then he came back in two months for a recheck, and there was an inescapable, incredible improvement. It just got better and better after that, with the tumor disappearing.”
“You could see it on the CAT scans,” says Doug. “There were no hot spots of cancer. And then, slowly but surely, you could see that the liver had started to grow back.” By February 2007, Doug was strong enough to overcome his final health obstacle: Surgeons at Northwestern removed the top part of his right lung, successfully ridding him of that tumor. Tests showed that the lung cancer had not spread to any other organs or lymph nodes.
“These kinds of stories are almost unheard of,” says Salem. “But in medicine, this is what we chase. We use statistics and clinical trials to help us try to make decisions, but what we are truly chasing with individualized patient care are these dramatic responses. It doesn’t mean that everyone is going to have this result, but it does show the proof of the concept. If we can fine-tune this therapy, then we can use it in so many ways.”
As for the Waldrons, they are understandably thrilled. “It’s a funny thing to say, given the circumstances,” Doug explains, “but it was a very good experience.” Diane adds, “They gave me my husband back.” Their future plans possibly include a move back to Arizona in the spring. “Why not?” Doug says. “I feel great.”
Photography: Tom Maday


