
It’s never too soon to worry about the sun’s effects. “The body remembers all of that ultraviolet radiation, from childhood on up,” cautions one dermatologist.
Each month over the past year, Orit Rindner, 46, has flown 6,000 miles from Tel Aviv to Chicago. Starting when she was seven, dozens of basal cell carcinomas have erupted on her face and scalp—so she happily makes the monthly trip to Northwestern University’s Feinberg School of Medicine to participate in a study of a pill that seems to shrink the growths. “Everything has disappeared,” she says.
Rindner suffers from a genetic condition called Gorlin syndrome, which makes her extremely susceptible to basal cell carcinomas. Without the medication, she would regularly need surgery to remove the growths. Like all drugs, the pink-and-gray pill, which is made by Genentech, carries a few side effects: Patients may lose hair, feel tired, or notice that food seems saltier and less tasty. So far, the pill appears to work for Rindner—although, she adds, “I don’t know the end of the story yet.”
After years of being overshadowed by breast cancer, skin cancer is finally getting, well, its day in the sun. (May, as it turns out, is Skin Cancer Awareness Month.) An estimated one in five Americans will develop some form of the disease, making it the most common form of cancer in the United States. More than two million U.S. residents get the disease each year, and the number is growing as more people are exposed to greater doses of ultraviolet light. Blame those Jersey Shore tans: More than 90 percent of nonmelanoma skin cancer is caused by too much ultraviolet radiation from the sun—and that’s without factoring in the effects of tanning booths.
Related:
Most people get basal cell carcinomas, which are rarely lethal, in the outer layer of the skin. (About 2,500 Americans die each year from squamous cell carcinomas, and another 8,000 from melanoma.) But patients suffering from basel cell carcinomas often have to undergo frequent surgeries, which can be disfiguring. This pill could offer them some hope. “We’re at the dawn of a new era for basal cell carcinoma with this drug,” says Simon Yoo, a Northwestern dermatologist and the lead investigator for the Chicago arm of the Genentech study.
Basal cell carcinomas typically look like small pearly pink pimples. Doctors are trying to get people to pay more attention to those innocuous-looking growths since they can get infected, spread into the eyes, and become significantly larger, growing downward into the muscle or bone or sideways into the cartilage of the nose. “In the olden days, it wasn’t uncommon to have very large lesions the size of a fist,” says Murad Alam, a dermatologic surgeon at Northwestern. (Though skin cancer is most common in fair-skinned people, Alam has treated Hispanics, Indians, Asians, and African Americans.)
The Genentech medication—which, until it gets approval from the Food and Drug Administration (FDA), goes by the names of Vismodegib and GDC-0449—blocks a receptor that signals cancer cells to proliferate. “It seems to make the cells start dying,” says Jennifer Low, an oncologist leading the development of Vismodegib at Genentech. By the end of the year, Genentech hopes to submit research to the FDA that shows how Vismodegib helps people with advanced basal cell carcinomas when surgery cannot remove them or would be disfiguring. Next up: a trial that evaluates the medicine’s effect on people whose basal cell carcinomas can be removed surgically.
Doctors are trying to perfect surgery that eliminates skin cancers without causing disfigurement. Currently, doctors remove cancerous lesions by burning or scraping them off. For less-operable forms of superficial basal cell carcinomas, they use radiation, light therapy, or Imiquimod, a topical cream that patients rub on the affected skin once a day for 8 to 16 weeks.
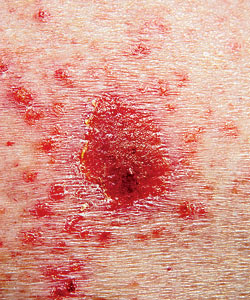
Basal cell carcinomas typically look like small pearly pink pimples.
The state-of-the-art treatment is Mohs surgery, named after its inventor, the Wisconsin doctor Frederick Mohs. Surgeons scoop out a tumor and the thin layer of tissue that surrounds it. They then look around the edges to see if any cancerous cells remain and keep cutting away until all the edges are clear. Doctors are also studying how optical imaging can help them see several layers deep into the skin before they make a cut. “But it’s not quite ready for prime time,” says Alam.
In addition, Northwestern researchers are seeking new ways to identify whether a bump is benign or malignant. (About 75,000 times a year, doctors aren’t sure.) Partnering with Abbott Labs and other institutions, they are working on a technique called fluorescent in situ hybridization, which looks at abnormalities in critical parts of DNA in hard-to-diagnose cases. “People send us samples from all over the country,” says Pedram Gerami, a Northwestern dermatologist at the Feinberg School of Medicine.
For the past two years, Northwestern—along with the University of California in San Francisco, Memorial Sloan-Kettering in New York, and a private lab in Irving, California—has also been using Abbott equipment with fluorescent “tags” to identify atypical, uncontrolled growth of cells on chromosomes 6 and 11. With information about changes in these areas, doctors are less likely to over- or undertreat patients. Researchers are also looking for changes on chromosome 8 that indicate how aggressively a tumor will grow.
Meanwhile, testing continues on Genentech’s Vismodegib. For some patients, FDA approval can’t come too soon. Over the past decade, George Chechopoulos has suffered through some two dozen surgeries to remove suspicious-looking basal cell carcinomas and moles. Now 56, the fair-skinned software engineer grew up getting blistering burns on the beach because he didn’t know better. “Ever since the experience of having these surgeries, I do wear sunscreen, a solid hat, and sunglasses all the time,” he says. But he also hopes the oral medication goes on the market so he can avoid further operations.
To sign up for the Genentech trial at Northwestern, call 312-695-6647.
Illustration: Michelle Thompson/agoodson.com


