Daru Smith was talking to his doctor and sister one day last December when he began to die. He saw their forms grow dim, a dark curtain coming down on them and himself in his fluorescent-lit hospital room at University of Chicago Medicine. Then the 29-year-old was above it all, looking into a hole in the ground where a torrent of water was swirling like a giant draining sink.
And then he was in a hallway. At the end of it glowed a white light. He felt at peace. No more heart palpitations, no flutters, no aches. He saw pictures on a wall. Scenes from his life. His son being born. Himself cutting the umbilical cord. Changing the baby’s diaper for the first time. He loved that child so much he’d given him his own name and called him Junior.
It felt good, the light. Until Daru realized: This is what happens when you die. He turned around and began to run. Faster. The scenes spooled past now. The light pulled him. I gotta fight.
Daru had been so sick. A few weeks earlier, he’d gone to the emergency room with a cold he couldn’t shake. But he knew it was more than that. He could barely keep up when his son, 3 years old by then, pedaled his bike ahead of him. And whenever Daru stepped from the cab of the 18-wheeler he drove for a living, he felt the world go sideways.
“You need to call your family,” the ER doctor had said when the test results came back. Daru had a bad case of pneumonia, but that wasn’t the worst. He was in cardiogenic shock, a condition in which the heart can’t pump enough blood to meet the body’s needs. If not treated immediately, Daru would die. What’s more, he also had something called sarcoidosis, a rare autoimmune disease that can cause the body to overproduce certain cells that infiltrate and all but shut down organs — in Daru’s case, the heart, liver, and kidneys.

That meant Daru needed all three vital organs replaced. That particular triple transplant is one of the rarest procedures in medicine, so complex and risky that it lies beyond the capacity of all but a handful of the nation’s elite hospitals. Only 15 had been performed.
Still unconscious, Daru continued to fight the light. Then his eyes fluttered and opened. “Hey, man, where did you go?” Daru’s cardiologist, Bryan Smith, said. “Thought we lost you for a second.”
In his white lab coat, his square jaw dusted with a light beard, the 36-year-old Smith could have stepped off the set of a medical soap. Seeing Daru on rounds every day, Smith had grown fond of him, admiring how hard he fought.
When he discovered that Daru had been approved for the triple transplant, Smith was thrilled but worried. If the operation came off, Daru would have a new life. But before it could even be attempted, he had to live long enough for a donor to be found. And not just any donor: one with three healthy organs compatible with Daru’s blood type — and sufficient to support his 6-foot-1 frame.
Daru’s close call that day wasn’t his first. He knew the light would be back.
Sarah McPharlin sat in a spare room at UChicago Medicine last November, waiting to plead for her life. She was there to meet with the center’s transplant evaluation team.
As different as Sarah was from Daru — the daughter of a special education teacher and a manager at Chrysler, she’d grown up in a tree-lined suburb of Detroit, gone to college and graduate school, traveled the world; he’d grown up as the fifth of seven children on the South Side, raised by a mother who managed a Harold’s Chicken Shack, where he worked until he found a better-paying job as a truck driver — they were, in more important ways, alike.
Like Daru, Sarah was 29. A rare autoimmune disease — in her case, an inflammatory condition called giant cell myocarditis — had attacked her heart. Complications from years of procedures and medications had all but destroyed her liver and kidneys. Her only hope, too, lay in a triple transplant.
Up until age 11, she seemed like a normal, healthy kid, smart (she was selected to give a speech at her fifth-grade graduation) and athletic (she played soccer and swam). It was while she was splashing in a pool, in fact, that a blinding headache seized her. She dipped her head in the water hoping it would offer relief. Moments later, her mother, Dianne, noticed her floating face-down. Sarah was rushed to a nearby hospital. Her heart had stopped, and a lifetime in and out of hospitals had begun.
Within a year, Sarah was stricken by a series of heart attacks. She had to be jump-started back to life again and again with defibrillator paddles. At 12, Sarah had a heart transplant, but over the years the replacement organ also began to fail. Surgeons had to open her chest five more times to repair ongoing problems.
By the time she and her mother traveled from their home in Grosse Pointe Woods, Michigan, to the October 2018 meeting at UChicago Medicine, her failing heart had led to such a buildup of fluid in her body that her shoes no longer fit. Her liver and kidneys had been damaged beyond repair. But the first few hospitals she approached for a triple transplant turned her down. It was too risky, they said. One predicted that she would die on the operating table.
Sarah discussed it with her family. She wasn’t ready to give up. In that case, the surgeon told her, there was one last place she could try.
Just outside the room where he was to meet Sarah McPharlin, Nir Uriel paused. As the UChicago Medicine heart specialist scanned her file, peering through his glasses at her history of surgeries and hospitalizations, he understood why she’d been turned down repeatedly.
Even without a tricky patient, triple transplants are difficult enough. They require a precisely timed orchestration of five surgeons — two taking out the donor organs at one hospital, three putting them in at another — each working with a team of nurses, anesthesiologists, and assistants.
The University of Pittsburgh’s Thomas Starzl, regarded as the father of modern transplants, oversaw the first heart-liver-kidney procedure in December 1989. The patient, Cindy Martin, didn’t make it to April. “They did everything they could,” her husband, John, told the New York Times. “They tried to make her life better. But she suffered for four months in the hospital and nothing was really accomplished.” Starzl, for all his towering accomplishments, was skeptical it could ever be done successfully.
It could, of course, but it would take 10 more years. It wasn’t until 1999 that UChicago Medicine performed the first successful heart-liver-kidney transplant — success here being defined by the patient living for at least a year. By the time Daru and Sarah were under consideration, UChicago Medicine had performed four of the 15 triple transplants of this kind ever undertaken.
It seemed unlikely that Sarah would be the 16th. The degree of difficulty of a heart transplant doubles with each previous cardiac operation. Sarah had undergone six: the initial transplant and five reparative surgeries. Those procedures had left her heart buried in scar tissue. This “hostile” chest, as surgeons call it, makes it harder for them to locate the arteries and veins they will need to disconnect and reattach. What’s more, she was so physically weak that doctors weren’t sure she could even survive such a grueling surgery.
There’s a macabre math that goes into such decisions. A triple transplant means using three organs that could potentially save three other patients. Does it make sense to use them on a single long shot?
Uriel’s first glimpse of the frail young woman that day only increased his skepticism. She was as pale as hospital sheets. She had almost no muscle mass. Her chest seemed to have collapsed in on itself, while fluid swelled her arms and abdomen. She could barely speak a sentence without gasping for breath.
Was she nervous? Uriel asked her. If UChicago Medicine turned her down, after all, she would be out of options.
“No,” she answered. “I’m not nervous. I’m full of hope.”
The optimism in her face moved Uriel.
What about her life posttransplant? What were her plans?
Her words spilled out in a giddy cascade. She’d travel, maybe back to Europe, where she had visited as a student ambassador in high school. She’d restart her career as an occupational therapist; she had earned her license but had practiced only three months before her health problems sidelined her. Beyond that? She loved spending time with her family. They were inseparable. Oh, and there would be Michigan State games! How could she forget about her alma mater?
“Could you excuse me for a minute?” Uriel said.
Just outside, he spoke to two colleagues, Gabriel Sayer, a heart failure specialist, and Catherine Murks, a nurse practitioner. “You have to meet this young woman,” Uriel said. They did, and saw what he saw: someone who, though facing death, radiated life.
Before the day was out, Sarah had gone from room to room talking to various members of the transplant evaluation team, telling and retelling her story to nearly 30 people. Afterward, they voted on whether to move forward. They gave a unanimous yes.
For both Sarah McPharlin and Daru Smith, it was now a waiting game. Waiting for organs to become available. Waiting, to put it in blunt terms, for the right person to die.
But there was also work to do. Work their lives depended on. Both had seized on their doctors’ orders to improve their strength for the surgeries — trudging quarter-mile laps around the intensive care unit, hoisting light weights.
Still, as November grayed into December, Daru’s doctors worried. His round face began to look drawn. Sullen silence replaced the jokes and easy banter the staff had come to expect. Some days, Bryan Smith would see his patient sweating, coughing, and lethargic, barely able to utter a complete sentence. Daru was wasting away before his eyes. The worst moments came when Daru would hover near death, seeing the light.
Daru had never been very religious, but he began to pray: I need those organs. If you’re up there, you need to show me something.
At his darkest point, a bright spot flickered: a friendship he’d struck up with a young woman two doors down in the ICU.
“Sarah,” she had said, introducing herself.
“I know,” Daru answered.
He had learned about her through his sister, who had chatted with Sarah’s mother in the hospital gym one day.
The attending physician for both, Smith had hoped they’d find each other. They would be uniquely able to understand what the other was going through and offer support. He would have made the introductions himself had it not been for an unwritten rule against doctors introducing transplant patients, even those not competing for the same organs.
Over the next weeks, a bond developed. Sarah and Daru compared notes on the paths that had led them here. In time, the two could be seen walking laps together, challenging each other on how many trips around the floor they could make, laughing at what they must look like in their gowns, with tubes and little machines trailing behind.
“You got this” became their go-to phrase.
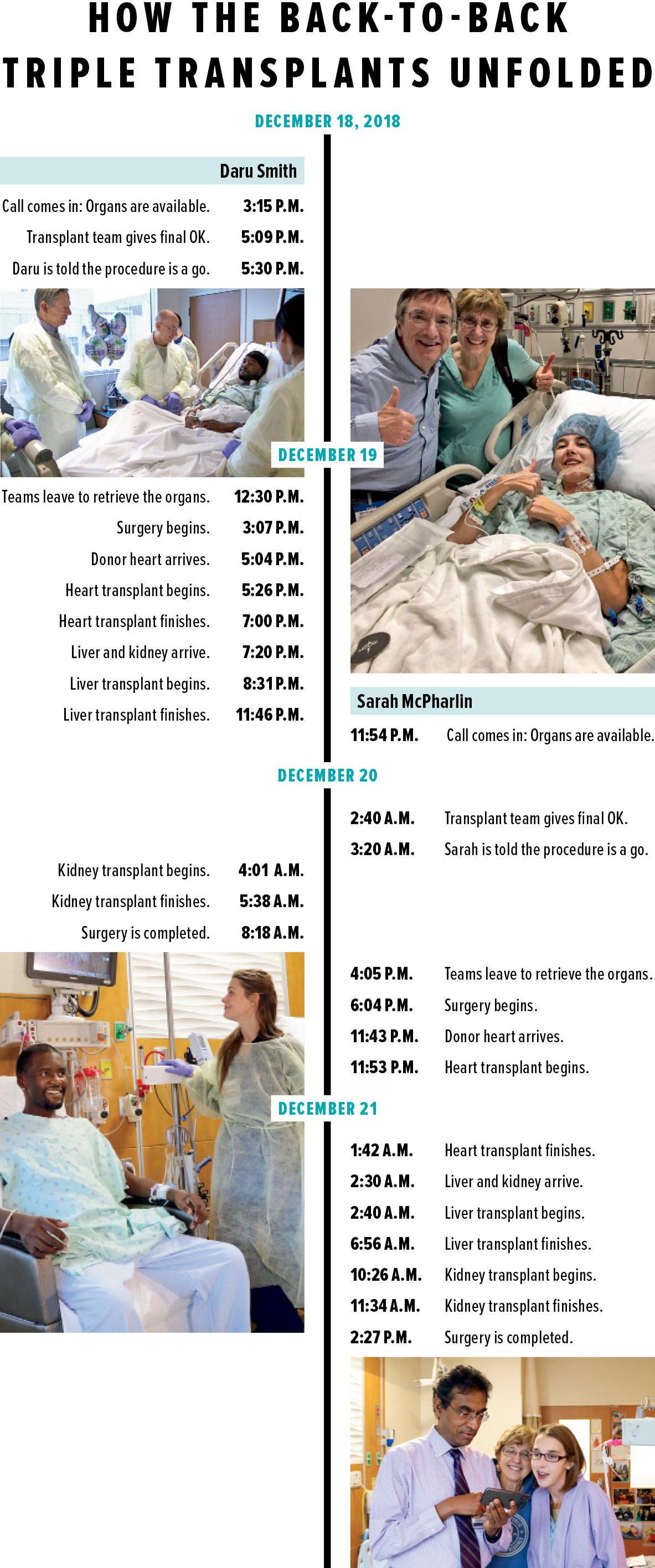
At 3:15 p.m. on Tuesday, December 18, the pager of Jamie Bucio, lead coordinator of UChicago Medicine’s organ procurement team, buzzed with an alert. A young man who was a potential match for Daru had been declared brain-dead. The man’s heart, liver, and kidneys were intact and strong, and his family had agreed to donate the organs.
Bucio is petite, voluble, and as efficient as a field commander, with a savant’s ability to summon names, dates, and patient histories at a moment’s notice. She leads a five-person team that arranges all the logistics involved in securing and transporting every one of the 180 or so organs transplanted each year at UChicago Medicine. On call 24 hours a day, she and her staff have one hour to respond with a preliminary acceptance once alerted to an available organ. Otherwise, it goes to the next patient on the waiting list.
Every moment of that hour is crucial. Bucio must first go online to evaluate the particulars of the organ: What kind of shape is it in? Is it a good match? Then she and her team alert the surgeons and the attending physician, sending them the particulars along with CT scans and other medical records of the patient. If everyone approves, then and only then is the patient notified that a transplant is a go — and will be happening in a matter of hours.

Immediately the procurement team begins making arrangements to retrieve the organ — booking slots in operating rooms at both hospitals and scheduling transportation. For the latter, Bucio turns to a contractor with a variety of aircraft waiting in a dedicated corner of Midway Airport. Depending on the distance, the trip may require a jet, prop plane, or helicopter. In this case, because the donor was within driving distance (UChicago Medicine asked that a specific location not be mentioned out of privacy concerns for the donor’s family), it meant three Chevrolet Suburbans.
After hearing back from all the surgeons, Bucio called the attending physician with the news: “Tell Daru it’s time.”
Smith in turn knocked on Daru’s ICU door, wearing a smile as he stepped inside. “You ready?”
“For what?”
“Are you ready?” Smith repeated.
Now Daru smiled, too.
“You’re not excited?” the cardiologist asked. “I thought you’d be jumping for joy.”
“I’m definitely excited,” Daru said. “Just not surprised.”
“Why not?”
“I called God out. I told him I needed my organs by the end of this week.”
“All right, then,” his doctor said with a laugh. “Let’s do this.”
At a glance, operating Room 5 West in UChicago Medicine’s Center for Care and Discovery is unremarkable. One of many similarly configured ORs, it sits at the end of a labyrinth of hallways on the sixth floor, filled with the most sophisticated medical equipment in the world. Giant wheels of light, attached to metal stanchions, flare onto the operating table, creating a center stage spotlight. On one wall, lines of red, yellow, and green blip across an enormous screen, each representing a different vital sign.
On most days, the immaculately clean white-tiled hallway just outside is deserted, save for the occasional appearance of a flock of surgeons, nurses, and orderlies, who enter, murmuring, the OR through a pair of double doors set in motion by the touch of a wall switch.
On this day, however — December 19, at a little before 3 in the afternoon — an unusually large contingent of 20 medical staff members milled about. The star of the show was the hospital’s head cardiac surgeon, Valluvan Jeevanandam. He’d be performing Daru’s heart transplant, the initial procedure upon which the rest of the undertaking rested.
Tall, lanky, and quick to smile, with threads of silver in his dark hair and the tapered fingers of classical pianist (or a heart surgeon), Jeevanandam was the ideal first baton carrier in a procedure that’s very much like a relay race: He handled the heart portion of the first successful triple transplant back in 1999. He was 39 at the time, a prodigy. Born in southern India, he had come to America as a young boy in a hurry. He skipped fifth grade, finished high school in three years, started college at 15, and graduated summa cum laude from Columbia University at 19. He had taken part in the other three triple transplants of this kind that UChicago Medicine had performed, too — in 2001, 2003, and 2011.
After scrubbing in, Jeevanandam’s team began prepping for the first leg of the marathon surgery that lay ahead. On one end of the room, a nurse neatly laid out a row of scalpels and hemostats on a metal tray and placed a chest spreader on a separate table. Meanwhile, the perfusionist set to his assigned task: readying the heart-lung bypass machine that would reroute Daru’s blood during the surgery.
Two floors below, in Daru’s ICU room, his family took turns saying a few words while Daru, already connected to IVs for the procedure, signed three sets of consent papers, one for each organ transplant. “Y’all gonna have to stop crying,” he said through his own tears. “Or I’m gonna have to put you out the room.”
While the family watched Daru being wheeled away, the three SUVs carrying the two surgical teams — one for the heart and one for the liver and kidney — sped across the city to retrieve the donor organs. The drivers — the transportation contractor tends to use retired police officers and firefighters — could use the sirens if necessary.
One reason for separate vehicles is expediency. A heart needs to be implanted within six hours — ideally within four hours — of being removed from a donor. So the heart team would return to UChicago Medicine immediately, while the liver and kidney team stayed behind to remove those organs.
Bucio ticked down her checklist of procurement tasks, including making sure the UChicago Medicine blood bank had an adequate supply of B-positive blood. One of the primary functions of the liver is to produce the coagulating substances that prevent excessive bleeding. With Daru’s liver already on the verge of a complete shutdown, there would be much blood lost.
To time the procedure as precisely as possible, Jeevanandam did not open Daru’s chest until the UChicago Medicine surgeon who had traveled to the other hospital began removing the donor’s heart. Once that happened, Jeevanandam stepped onto a black spongy mat in his track shoes — which he always wears for comfort during long procedures — and made his first cut at 3:07 p.m.
Inserting the rib spreader, a stainless steel retractor used to lay bare the chest cavity, Jeevanandam began to slowly crank. Daru was then hooked up to the heart-lung bypass machine, the major arteries to his heart clamped shut, leaving Daru without a functioning heart for what would be 102 minutes, and began the removal process. The donor organ, packed in a Tupperware pickle jar, bathed in a preservation solution, and chilled in a medical box similar to an Igloo cooler, arrived at 5:04 p.m.
Daru’s sarcoidosis presented a complication for Jeevanandam. A healthy person’s tissue is like supple leather, which helps it fuse when sewn together. Much of Daru’s tissue was more like cardboard, so Jeevanandam had to be extra careful not to rip it while sewing in the new heart.
That accomplished, Daru was ready to be taken off the bypass machine. In transplant surgery, it is always a tense moment when the aortic clamp is removed. To preserve a heart for transport, doctors fill it with a solution high in potassium. If all goes well, when the clamp is released, the whoosh of blood into the heart restores normal levels of potassium and other electrolytes, and the heart begins to beat.
That does not always happen, though. Sometimes, the heart will start fibrillating and need a shock. Other times, it won’t beat at all and the surgeon has to “tickle” it to life, as Jeevanandam puts it. That was the case with Daru.
Using forceps, Jeevanandam gently massaged the heart until, finally, a dot began to hop up from the long flat green line on the screen across the room. With that, Jeevanandam stepped back, his gloved hands raised. His part was done. It was 7:00 p.m.
As his assistants spent the next hour or so affixing drainage tubes and packing the area around the heart with gauze to absorb blood, Talia Baker, the surgeon performing the liver transplant, and her team were already setting up.
Performing a Liver transplant is a lot like plumbing. There are some 180 steps, but basically the surgeon has to plug in the four main pipes that allow a flow into and out of the organ: the portal vein, through which the liver gets three-quarters of its blood; the hepatic artery, which feeds blood to the bile duct; the bile duct itself, which moves that digestive aid from the liver into the small intestine; and the vena cava, where blood flows into the liver from the lower body and out into the heart.
Baker faced an extra challenge with Daru. A healthy liver has the spongy consistency of a jellyfish, which makes it pliable. A cirrhotic, or scarred, liver like Daru’s is firm, so manipulating it is more difficult, raising the risk of damage to the organ.
Just as the transplant of a heart has its moment of truth — whether the new organ starts beating when the clamp is removed — so does one of a liver. A long absence of the oxygen and nutrients that blood supplies can make the new organ susceptible to severe damage once the blood flow is restored. That damage can even cause the heart and lungs to collapse, resulting in instant death. It’s rare, occurring in only 1 percent of liver transplants, but the possibility still gives surgeons pause when unclamping the major vessels. In Daru’s case, though, the new liver handled the blood flow as it was supposed to.
At 11:46 p.m., the second portion of his transplant was complete. All that was left: the kidney.
Eight minutes later, as baker’s assistants were finishing up with Daru, Bucio got a page that stunned her: A young woman in another state had been declared brain-dead. She was a potential match for Sarah, and she had three healthy organs. Was UChicago Medicine interested?
Bucio called Bryan Smith, Sarah’s attending physician. “Well, I guess nobody’s getting any sleep for the next 48 hours,” she said.
“What are you talking about?” Smith responded.
“Sarah,” she explained. “We have an offer.”
“You’re kidding?”
Smith soon found himself, for the second time in two days, knocking on a patient’s door with life-altering news.
A month earlier, not long after she’d been admitted, Sarah had endured a false start. The transplant team’s members believed they had organ matches, and she was already in an operating room when word came that there was a problem with the heart. The surgery was off. It was a hugely disappointing turn of events for her and her family.
Smith felt sure that wasn’t going to happen again. He’d seen the charts of the donor patient. Her organs were in perfect shape. Still, he forced himself not to get too excited when he entered her room, where the family appeared to be celebrating.
“So you’ve heard the news?” he asked.
“Yeah,” said Sarah. “Daru got his organs and his surgery is going really well!”
“No, no, we actually have an offer for you.”
Sarah stared at him in disbelief.
She wasn’t the only one having a hard time fathoming what was happening. No hospital had ever performed two triple transplants within a year. UChicago Medicine was preparing to begin a second one within 27 hours of starting the first. Was that even possible? It had to be. The offer of three matching organs simply could not be turned down.
Bucio had already sprung into action, working out the logistics. Because Sarah’s organs were coming from some distance, UChicago Medicine would need two jets, plus ground transportation to and from both airports.
Meanwhile, the cell phones of surgeons, nurses, anesthesiologists, and assistants were lighting up with group texts. “It’s all hands on deck,” Bucio told her team.
Less than 24 hours earlier, Yolanda Becker, director of UChicago Medicine’s kidney and pancreas program, had been starting her Christmas staycation, with plans to go to a spin class, spend time with her family, maybe pamper herself a little. Then came the call about Daru. The hospital’s only other kidney transplant surgeon, Piotr Witkowski, would be retrieving the donor organ. Could Becker put in Daru’s new kidney? “Of course,” she had said.
Now she would be doing Sarah’s, too.
For some members of the surgical teams, the two procedures would mean not just being awake but working for up to two days straight. But doctors are used to taxing stints. Over the years, Becker has learned to nap standing up. Jeevanandam, the heart surgeon for both transplants, once flew to India, spent a few hours lecturing students shortly after he landed, performed a transplant, went to dinner, and caught a plane back to Chicago — all with no sleep.
For months, the staff had gone over the logistics of pulling off a triple transplant. But the uncharted ground of a second one presented unforeseen complications. Becker worried she might not have enough sterilized instruments on hand. Altogether, the surgeons would need some 600 to 700 instruments for each of the two triple transplants. There were also three other transplants happening at the hospital at this time, one of which was a double: kidney and liver.
In between each use, instruments have to be taken to a sterilizing area to be washed and inspected before they are loaded into a special sterilization machine. After that, the instruments are inspected again and assembled onto trays, each of which holds about 100 tools. Those trays are wrapped and boxed, then loaded into an autoclave, a pressure cooker of sorts that uses steam to kill microorganisms resistant to detergent and boiling water. The entire process takes three hours.
To ensure that Becker and the other surgeons had the instruments they needed when they needed them, the sterilization team would monitor a giant scoreboard-like screen that tracks what stage every surgery is in. They would give the tools of the triple transplant surgeons top priority.
At 8:18 a.m. on December 20, his triple transplant completed after more than 17 hours in surgery, Daru was moved back to the ICU. Less than 10 hours later, and in the same operating room, Sarah’s triple transplant began.
As Jeevanandam had anticipated, the heart portion of her surgery required extra care, taking nearly twice as long as Daru’s. The scar tissue that had built up in her chest from past surgeries made hunting for all the arteries and veins like an archaeological dig. Just as an archaeologist uses little brushes to carefully clear away dust and debris, Jeevanandam had to use special instruments to tease apart the tissue to find the arteries underneath. A single millimeter miscalculation with a scalpel could cause a nick in the heart itself.
Sarah’s liver posed special challenges, as well. Because she had been on immunosuppressive drugs for most of her life, her tissues were extremely fragile. Baker had to work slowly and precisely, taking painstaking care with each incision and suture.
Becker was last up. And as the final surgeon, she had to not only perform the kidney transplant but also make sure the heart and liver were still functioning, which meant keeping a close eye on all of Sarah’s vital signs. She also had to navigate the minefield of drains and chest tubes and pacemaker wires left in place by the previous two surgeons. Dislodge any of the tubes or drains and she could miss internal bleeding. Detach a pacemaker wire and the heart could develop a dangerous arrhythmia without her knowing.
By the time her surgery was done, at 2:27 p.m. on Friday, Sarah had been on the table for more than 20 hours.
“We never in our wildest dreams imagined both would take place at virtually the same time,” John Fung, codirector of UChicago Medicine’s Transplant Institute and a protégé of triple-transplant pioneer Thomas Starzl, said at a press conference on January 4. “Pulling this off can feel like trying to perform a high-wire ballet in the middle of running a marathon.”
Just days after the surgery, Sarah was amazed by how good she felt. Before the transplant, she had gained 45 pounds of water weight. It was nice to have her normal legs again. She’d also felt out of breath and cold all the time, a result of the poor circulation caused by her failing heart. Now she didn’t have to constantly swaddle herself in a blanket or coat.
Her and Daru’s recoveries have not been without complications. In January, tests revealed that Daru’s liver enzymes were elevated, so surgeons placed a stent in one of his bile ducts to open up a blocked passageway. He also got an infection, which was cleared up with antibiotics.
In Sarah’s case, physicians noticed some blood in one of the drains inserted near her liver. The only way to rule out a problem was to return her to the OR. And since her discharge, 17 days after the transplant, Sarah has registered low magnesium levels, requiring weekly infusions of the mineral, which keeps the heartbeat steady and maintains nerve and muscle functions. She’s also struggled at times with a low white blood cell count, necessitating booster shots, and painful shin splints in her left leg, likely the result of years of taking anti-inflammatory medication.
The issues have forced her to use a wheelchair on some family outings, but she has gone nonetheless — to Northwestern’s Cancer Survivors’ Celebration Walk in Grant Park, to PorchFest Lakeview, to fireworks at Navy Pier. And they have not caused her to give up on a goal she set when she heard she’d be getting new organs: competing in the Transplant Games of America, which will take place next July at the New Jersey Meadowlands.
She also plans to fulfill a pact. While she and Daru were waiting for their organs, she told her new friend that when it was all done, when both of them had their new organs, they should meet up in a sunny place, maybe at Millennium Park or by the lake. Maybe she and her mother could take him to dinner. She would like to meet his son. Daru laughed and said, “I’m a vegan now.” Sarah smiled back. “Vegan it is.”
A few days after Sarah’s discharge, Daru was granted his own release from the hospital he’d called home for eight weeks. Wearing a paper mask to guard against infection and balancing a large poster card filled with well wishes, he was wheeled through the ICU toward the elevator, bound for the garage where his sister was waiting.
Along the way, nurses, doctors, and administrative staff clapped and waved and shouted goodbyes.
“Thank you,” he said back, his voice still raspy from the recently removed breathing tube. “Thank you for everything.”
“You are loved here,” the orderly pushing his wheelchair said.
They turned one corner. And then another.
And then they stood looking down a final hallway. At the end of it shone what looked like a bright white light.
The orderly pushed him forward. And as he did, the source became clear: a set of white double doors illuminated by bright discs of light in the ceiling. The white grew brighter and brighter until Daru was suddenly on the other side, where he saw a familiar car and his sister standing beside it, smiling, waiting to take him home to his son.



